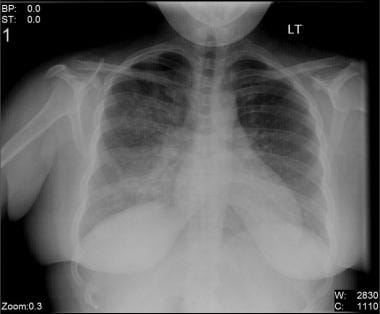 
Streptococcal pneumonia in a 35-year-old patient. Centrilobular nodules, bronchial wall thickening, and bronchiectasis are seen in patients who are concurrently infected with other organisms. A small amount of reactive pleural effusion is usually seen. Patchy areas of consolidation that may be multilobar or bilateral have been seen in patients, following antibiotic therapy. The lung volume is not altered, and cavitation is rare. It predominantly involves lower lobes ( Figure 1). Lobar pneumonia is the most common imaging appearance. Streptococcus pneumonia is the most common aetiological agent producing CAP. The cause of aspiration pneumonias are micro-organisms that colonise the oropharynx these include Gram-positive cocci, Gram-negative rods, and anaerobic bacteria. Aerobic Gram-negative bacilli, particularly Pseudomonas aeruginosa and Enterobacteriae and a few Gram-positive cocci such as Staphylococcus aureus are more commonly responsible for hospital-acquired pneumonia (HAP). The most common causes of community-acquired pneumonia (CAP) are Streptococcus pneumonia, Haemophilus influenzae, Mycoplasma pneumoniae, Chlamydia pneumoniae, and Legionella pneumophila. In the current era, pneumonias are preferably classified as community-acquired, nosocomial, or aspiration pneumonia, depending on their origin. This classification is no longer commonly used because, with new organisms and widespread use of antibiotics, morphological patterns nowadays are mostly overlapping. Interstitial pneumonia is caused by the involvement of bronchial or bronchiolar wall and pulmonary interstitium and leads to septal thickening, nodules, and areas of ground glass opacities (GGO) on imaging. In bronchopneumonia, there are centrilobular nodules that coalesce to cause consolidation, and involve one or more lobes. Lobar consolidation is characterised by confluent areas of consolidation, which are usually confined to one segment or lobe. 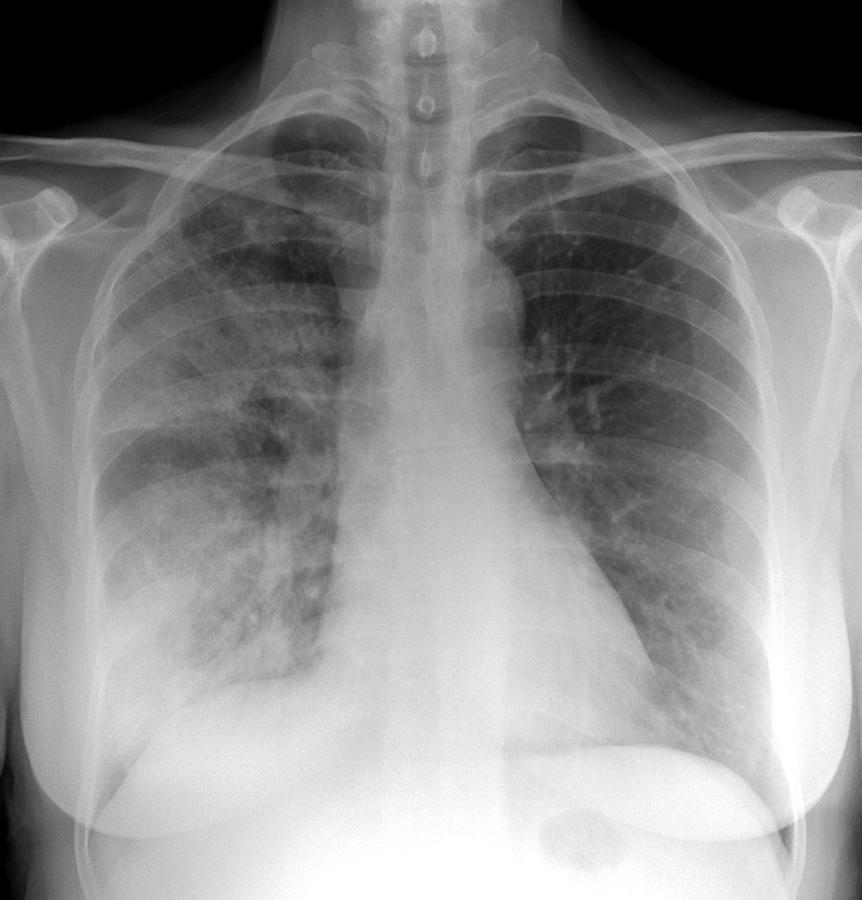
Pneumonia was classically divided according to its morphological pattern on imaging into the following: lobar pneumonia, bronchopneumonia, and interstitial pneumonia. Recently, data has been published regarding the utility of magnetic resonance imaging (MRI) as a radiation-free technique for diagnosing pulmonary infections. The main role of chest ultrasonography in pneumonia is to assess pleural effusion or empyema and serve as a guide for aspiration/drainage. It is not used for the initial evaluation of pneumonia but may be used when the response to treatment is unusually slow, to look for complications, to detect underlying disease within the lung, and also to characterise any complex pneumonias. CT may detect abnormalities that are not appreciable on chest radiograph. It can also diagnose complications like pleural effusion, pneumothorax, and abscess formation. A chest radiograph can establish the presence of pneumonia, determine its extent and location, and assess the response to treatment. Ĭhest radiographs are the most widely used imaging modality followed by cross-sectional imaging methods like computed tomography (CT). However, the term ‘pneumonia’ usually refers to infection by a pathogenic organism, which results in consolidation of the lung, whereas the term pneumonitis is generally used in the context of non-infective inflammation that primarily involves the alveolar wall. Pneumonitis and pneumonia are terms that refer to a similar pathology and can be used interchangeably. Pneumonia is defined as an infection of the lower respiratory tract, which involves the lung parenchyma.
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
